 | |
| Clinical data | |
|---|---|
| Trade names | Survector, others |
| Other names | S-1694 |
|
Routes of administration | Oral |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Metabolism | Hepatic |
| Elimination half-life | Amineptine: 0.8–1.0 hours
[2]
[3] Metabolite: 1.5–2.5 hours [2] [3] |
| Excretion | Renal |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard ( EPA) | |
| ECHA InfoCard | 100.055.271 |
| Chemical and physical data | |
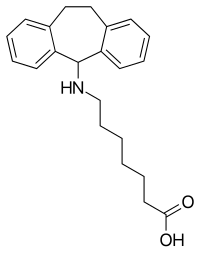
| Formula | C22H28NO2 |
| Molar mass | 338.471 g·mol−1 |
| 3D model ( JSmol) | |
| |
| |
| (verify) | |
Amineptine, formerly sold under the brand name Survector among others, is an atypical antidepressant of the tricyclic antidepressant (TCA) family. [4] [5] It acts as a selective and mixed dopamine reuptake inhibitor and releasing agent, and to a lesser extent as a norepinephrine reuptake inhibitor. [4] [5]
Amineptine was developed by the French Society of Medical research in the 1960s. [6] Introduced in France in 1978 by the pharmaceutical company Servier, [7] amineptine soon gained a reputation for abuse due to its short-lived, but pleasant, stimulant effect experienced by some patients.
After its release into the European market, cases of hepatotoxicity emerged, some serious. This, along with the potential for abuse, led to the suspension of the French marketing authorization for Survector in 1999. [8]
Amineptine is illegal in both Germany and the United States.
Medical uses
Amineptine was approved in France for severe clinical depression of endogenous origin in 1978. [9]
Contraindications
- Chorea
- Hypersensitivity: Known hypersensitivity to amineptine, in particular antecedents of hepatitis after dosage of the product.
- MAO inhibitors
Precautions for use
Warnings and precautions before taking amineptine: [10]
- Breast feeding
- Children less than 15-year of age
- General anaesthesia: Discontinue the drug 24 to 48 hours before anaesthesia.[ citation needed]
- Official sports/
Olympic Games: Prohibited substance.
- 7 March Official Journal 2000.
- Pregnancy (first trimester)[ citation needed]
Effects on the fetus
- Lacking information in humans
- Non- teratogenic in rodents
Side effects
Dermatological
Severe acne due to amineptine was first reported in 1988 by various authors—Grupper, Thioly-Bensoussan, Vexiau, Fiet, Puissant, Gourmel, Teillac, Levigne, to name a few—simultaneously [11] [12] [13] [14] [15] in the same issue of Annales de Dermatologie et de Vénéréologie and in the 12 March 1988 issue of The Lancet. [16] A year later, Dr Martin-Ortega and colleagues in Barcelona, Spain reported a case of "acneiform eruption" in a 54-year-old woman whose intake of amineptine was described as "excessive." [17] One year after that, Vexiau and colleagues reported six women, one of whom never admitted to using amineptine, getting severe acne concentrated in the face, back and thorax, the severity of which varied with the dosage. [18] Most of them were treated unsuccessfully with isotretinoin (Accutane) for about 18 months; two of the three that discontinued amineptine experienced a reduction in cutaneous symptoms, with the least affected patient going into remission. [18]
Psychiatric
Psychomotor excitation can very rarely occur with this drug.
- Insomnia
- Irritability
- Nervousness
- Suicidal ideation. Seen early in the treatment, by lifting of psychomotor inhibition.
Abuse and dependence
The risk of addiction is low, but exists nonetheless. Between 1978 and 1988, there were 186 cases of amineptine addiction reported to the French Regional Centres of Pharmacovigilance; an analysis of 155 of those cases found that they were predominantly female, and that two-thirds of cases had known risk factors for addiction. [19] However, a 1981 study of known opiate addicts and schizophrenia patients found no drug addiction in any of the subjects. [20] In a 1990 study of eight amineptine dependence cases, the gradual withdrawal of amineptine could be achieved without problems in six people; in two others, anxiety, psychomotor agitation, and/or bulimia appeared. [21]
Withdrawal
Pharmacodependence is very common with amineptine compared to other antidepressants. [22] A variety of psychological symptoms can occur during withdrawal from amineptine, [23] such as anxiety and agitation. [24]
Cardiovascular
Very rarely:
Hepatic
Amineptine can rarely cause hepatitis, of the cytolytic, cholestatic varieties. [25] Amineptine-induced hepatitis, which is sometimes preceded by a rash, is believed to be due to an immunoallergic reaction. [26] It resolves upon discontinuation of the offending drug. [25] The risk of getting this may or may not be genetically determined. [27]
Additionally, amineptine is known to rarely elevate transaminases, alkaline phosphatase, and bilirubin. [28]
Mixed hepatitis, which is very rare, generally occurs between the 15th and 30th day of treatment. Often preceded by sometimes intense abdominal pains, nausea, vomiting or a rash, the jaundice is variable. Hepatitis is either of mixed type or with cholestatic prevalence. The evolution was, in all the cases, favorable to the discontinuation of the drug. The mechanism is discussed (immunoallergic and/or toxic). [29]
In circa 1994 Spain, there was a case associating acute pancreatitis and mixed hepatitis, after three weeks of treatment. [30]
Lazaros and colleagues at the Western Attica General Hospital in Athens, Greece reported two cases of drug induced hepatitis 18 and 15 days of treatment. [31]
One case of cytolytic hepatitis occurred after ingestion of only one tablet. [32]
Gastrointestinal
- Acute pancreatitis (very rare) A case associating acute pancreatitis and mixed hepatitis after three weeks of treatment. [30]
Immunological
In 1989, Sgro and colleagues at the Centre de Pharmacovigilance [33] in Dijon reported a case of anaphylactic shock in a woman who had been taking amineptine. [34]
Pharmacology
Pharmacodynamics
| Site | Ki (nM) | Species | Ref |
|---|---|---|---|
| SERT | >100,000 ( IC50) | Rat | [36] |
| NET | 10,000 (IC50) 3,560 |
Rat Canine |
[36]
[37] [38] |
| DAT | 1,000–1,400 (IC50) 3,330 |
Rat Canine |
[36]
[39]
[37] [38] |
| 5-HT1A | >100,000 | Rat | [40] |
| 5-HT2A | 74,000 | Rat | [40] |
| α1 | >100,000 | Rat | [40] |
| α2 | >100,000 | Rat | [40] |
| β | >100,000 | Rat | [40] |
| D1 | >100,000 | Canine | [36] |
| D2 | >100,000 | Rat/canine | [36] [40] |
| H1 | >100,000 13,000 |
Rat Guinea pig |
[40] [41] |
| mACh | >100,000 | Rat | [40] |
| Values are Ki (nM), unless otherwise noted. The smaller the value, the more strongly the drug binds to the site. | |||
Amineptine inhibits the reuptake of dopamine and, to a much lesser extent, of norepinephrine. [37] [36] [42] In addition, it has been found to induce the release of dopamine. [37] [36] [42] However, amineptine is much less efficacious as a dopamine releasing agent relative to D-amphetamine, and the drug appears to act predominantly as a dopamine reuptake inhibitor. [37] [36] [42] In contrast to the case for dopamine, amineptine does not induce the release of norepinephrine, and hence acts purely as a norepinephrine reuptake inhibitor. [37] [36] [42] Unlike other TCAs, amineptine interacts very weakly or not at all with the serotonin, adrenergic, dopamine, histamine, and muscarinic acetylcholine receptors. [40] [41] [42] The major metabolites of amineptine have similar activity to that of the parent compound, albeit with lower potency. [42]
No human data appear to be available for binding or inhibition of the monoamine transporters by amineptine. [43]
Pharmacokinetics
Peak plasma levels of amineptine following a single 100 mg oral dose have been found to range between 277 and 2,215 ng/mL (818–6,544 nM), with a mean of 772 ng/mL (2,281 nM), whereas maximal plasma concentrations of its major metabolite ranged between 144 and 1,068 ng/mL (465–3,452 nM), with a mean of 471 ng/mL (1,522 nM). [2] After a single 200 mg oral dose of amineptine, mean peak plasma levels of amineptine were around 750 to 940 ng/mL (2,216–2,777 nM), while those of its major metabolite were about 750 to 970 ng/mL (2,216–3,135 nM). [3] The time to peak concentrations is about 1 hour for amineptine and 1.5 hours for its major metabolite. [2] [3] The elimination half-life of amineptine is about 0.80 to 1.0 hours and that of its major metabolite is about 1.5 to 2.5 hours. [2] [3] Due to their very short elimination half-lives, amineptine and its major metabolite do not accumulate significantly with repeated administration. [2]
Society and culture
Brand names
Amineptine has been sold under a variety of brand names including Survector, Maneon, Directim, Neolior, Provector, and Viaspera.
Legal status
It had been proposed that Amineptine become a Schedule I controlled substance in the United States in July 2021. [44] This announcement was followed by the placement of Amineptine into Schedule I. [45]
References
- ^ Anvisa (31 March 2023). "RDC Nº 784 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 784 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 4 April 2023). Archived from the original on 3 August 2023. Retrieved 16 August 2023.
- ^ a b c d e f Lachatre G, Piva C, Riche C, et al. (1989). "Single-dose pharmacokinetics of amineptine and of its main metabolite in healthy young adults". Fundam Clin Pharmacol. 3 (1): 19–26. doi: 10.1111/j.1472-8206.1989.tb00026.x. PMID 2714729. S2CID 25992333.
- ^ a b c d e Sbarra C, Castelli MG, Noseda A, Fanelli R (1981). "Pharmacokinetics of amineptine in man". Eur J Drug Metab Pharmacokinet. 6 (2): 123–6. doi: 10.1007/bf03189478. PMID 7274306. S2CID 31069503.
- ^ a b Vaugeois JM, Corera AT, Deslandes A, Costentin J (June 1999). "Although chemically related to amineptine, the antidepressant tianeptine is not a dopamine uptake inhibitor". Pharmacology Biochemistry and Behavior. 63 (2): 285–90. doi: 10.1016/S0091-3057(98)00242-1. PMID 10371658. S2CID 32862145.
- ^ a b Dunlop BW, Nemeroff CB (2007). "The role of dopamine in the pathophysiology of depression". Arch. Gen. Psychiatry. 64 (3): 327–37. doi: 10.1001/archpsyc.64.3.327. PMID 17339521. S2CID 26550661.
- ^ DE Patent 2011806 – NEW TRICYCLIC DERIVATIVES AND PROCESS FOR THEIR MANUFACTURE
- ^ Sittig M (1 April 1988) [1979]. Pharmaceutical Manufacturing Encyclopedia (2nd ed.). Park Ridge, New Jersey, United States American: William Andrew Publishing/Noyes Publications. ISBN 978-0-8155-1144-1. Archived from the original on 23 October 2005. Retrieved 29 October 2005.[ page needed]
- ^ "Docket No. 02N-0101". U.S. Food and Drug Administration. 9 April 2002. Retrieved 30 January 2014.
- ^ Doctissimo (2005). "SURVECTOR – Amineptine" (in French). Archived from the original on 9 March 2005. Retrieved 27 October 2005.
- ^ Amineptine Medication – Uses, Side Effects and Precautions of Amineptine. Health-care-information.org. Retrieved on 28 September 2013
- ^ Grupper C (1988). "[New iatrogenic acne: acne caused by amineptin (Survector)]". Annales de Dermatologie et de Vénéréologie (in French). 115 (11): 1174–6. PMID 2977079.
- ^ Thioly-Bensoussan D, Charpentier A, Triller R, et al. (1988). "[Iatrogenic acne caused by amineptin (Survector). Apropos of 8 cases]". Annales de Dermatologie et de Vénéréologie (in French). 115 (11): 1177–80. PMID 2977080.
- ^ Vexiau P, Gourmel B, Husson C, et al. (1988). "[Severe lesions of acne type induced by chronic amineptin poisoning: apropos of 6 cases]". Annales de Dermatologie et de Vénéréologie (in French). 115 (11): 1180–2. PMID 2977081.
- ^ Teillac D, Weber MJ, Lowenstein W, de Prost Y (1988). "[Acne caused by Survector]". Annales de Dermatologie et de Vénéréologie (in French). 115 (11): 1183–4. PMID 2977082.
- ^ Lévigne V, Faisant M, Mourier C, et al. (1988). "[Monstrous acne in the adult. Inducer role of Survector?]". Annales de Dermatologie et de Vénéréologie (in French). 115 (11): 1184–5. PMID 2977083.
- ^ Vexiau P, Gourmel B, Julien R, et al. (March 1988). "Severe acne-like lesions caused by amineptine overdose". Lancet. 1 (8585): 585. doi: 10.1016/S0140-6736(88)91373-6. PMID 2894512. S2CID 32936080.
- ^ Martín-Ortega E, Zamora E, Herrero C, Palou J (1989). "[Acneiform eruption induced by amineptin (Survector)]". Medicina Cutánea Ibero-latino-americana (in Spanish). 17 (6): 414–6. PMID 2534534.
- ^ a b Vexiau P, Gourmel B, Castot A, et al. (1990). "Severe acne due to chronic amineptine overdose". Archives of Dermatological Research. 282 (2): 103–7. doi: 10.1007/BF00493467. PMID 2141246. S2CID 39394890.
- ^ Castot A, Benzaken C, Wagniart F, Efthymiou ML (1990). "[Amineptin abuse. Analysis of 155 cases. An evaluation of the official cooperative survey of the Regional Centers of Pharmacovigilance]". Thérapie (in French). 45 (5): 399–405. PMID 2260032.
- ^ Deniker P, Lôo H, Zarifian E, et al. (1981). "[Amineptine and amotival syndrome (author's transl)]". L'Encéphale (in French). 7 (1): 59–64. PMID 7227285.
- ^ Bertschy G, Luxembourger I, Bizouard P, Vandel S, Allers G, Volmat R (1990). "[Amineptin dependence. Detection of patients at risk. Report of 8 cases]". L'Encéphale (in French). 16 (5): 405–9. PMID 2265603.
- ^ Blayac JP, Hillaire-Buys D, Peyrière H (1997). "[Pharmacovigilance of new antidepressants: evaluation of neuro-psychobehavioral disorders]". Thérapie. 52 (2): 117–22. PMID 9231505.
- ^ Castot A, Benzaken C, Wagniart F, Efthymiou ML (1990). "[Amineptin abuse. Analysis of 155 cases. An evaluation of the official cooperative survey of the Regional Centers of Pharmacovigilance]". Thérapie. 45 (5): 399–405. PMID 2260032.
- ^ Bertschy G, Luxembourger I, Bizouard P, Vandel S, Allers G, Volmat R (1990). "[Amineptin dependence. Detection of patients at risk. Report of 8 cases]". L'Encéphale. 16 (5): 405–9. PMID 2265603.
- ^ a b Bories P, Pomier-Layrargues G, Chotard JP, et al. (December 1980). "[Amineptine-induced cholestatic hepatitis. 5 cases (author's transl)]". La Nouvelle Presse Médicale (in French). 9 (48): 3689–92. PMID 7454584.
- ^ Pessayre D, Larrey D (April 1988). "Acute and chronic drug-induced hepatitis". Baillière's Clinical Gastroenterology. 2 (2): 385–422. doi: 10.1016/0950-3528(88)90009-7. PMID 3044468.
- ^ Larrey D, Pageaux GP (1997). "Genetic predisposition to drug-induced hepatotoxicity". Journal of Hepatology. 26 (Suppl 2): 12–21. doi: 10.1016/S0168-8278(97)80492-8. PMID 9204405.
- ^ "Questions au Professeur Daniel Dhumeaux" [Drug-induced liver disorders. Questions for Professor Daniel Dhumeaux]. Gastroentérologie Clinique et Biologique (in French). 23 (8–9): 917–20. 1999. PMID 10533145.
- ^ Concours Med 1982; 104:5733-5734[ verification needed]
- ^ a b Sebastián Domingo JJ, Simón Marco MA, Uribarrena Echebarría R (March 1994). "Hepatic and pancreatic injury associated with amineptine therapy". Journal of Clinical Gastroenterology. 18 (2): 168–9. doi: 10.1097/00004836-199403000-00023. PMID 8189020.
- ^ Lazaros GA, Stavrinos C, Papatheodoridis GV, Delladetsima JK, Toliopoulos A, Tassopoulos NC (1996). "Amineptine induced liver injury. Report of two cases and brief review of the literature". Hepato-gastroenterology. 43 (10): 1015–9. PMID 8884331.
- ^ Jonville AP, Dutertre JP, Autret E (1992). "[Immediate acute hepatic cytolysis after the administration of a single amineptin tablet]". Gastroentérologie Clinique et Biologique (in French). 16 (4): 368. PMID 1397859.
- ^ centres-pharmacovigilance.net Archived 8 February 2012 at the Wayback Machine
- ^ Sgro C, Lacroix S, Waldner A, Lacroix M, Ferrut O, Bureau A (1989). "[Anaphylactic shock caused by amineptine. Report of a case]". La Revue de Médecine Interne (in French). 10 (5): 461–2. doi: 10.1016/s0248-8663(89)80054-2. PMID 2488491.
- ^ Roth BL, Driscol, J. "PDSP Ki Database". Psychoactive Drug Screening Program (PDSP). University of North Carolina at Chapel Hill and the United States National Institute of Mental Health. Retrieved 14 August 2017.
- ^ a b c d e f g h i Garattini S, Mennini T (1989). "Pharmacology of amineptine: synthesis and updating". Clin Neuropharmacol. 12 (Suppl 2): S13–8. doi: 10.1097/00002826-198912002-00003. PMID 2698268. S2CID 10947713.
- ^ a b c d e f Ceci A, Garattini S, Gobbi M, Mennini T (1986). "Effect of long term amineptine treatment on pre- and postsynaptic mechanisms in rat brain". Br. J. Pharmacol. 88 (1): 269–75. doi: 10.1111/j.1476-5381.1986.tb09495.x. PMC 1917102. PMID 3708219.
- ^ a b Nishino S, Mao J, Sampathkumaran R, Shelton J (1998). "Increased dopaminergic transmission mediates the wake-promoting effects of CNS stimulants". Sleep Res Online. 1 (1): 49–61. PMID 11382857.
- ^ Protais P, Arbaoui J, Bakkali EH, Bermejo A, Cortes D (1995). "Effects of various isoquinoline alkaloids on in vitro 3H-dopamine uptake by rat striatal synaptosomes". J. Nat. Prod. 58 (10): 1475–84. doi: 10.1021/np50124a001. PMID 8676127.
- ^ a b c d e f g h i Hall H, Sällemark M, Wedel I (1984). "Acute effects of atypical antidepressants on various receptors in the rat brain". Acta Pharmacol Toxicol (Copenh). 54 (5): 379–84. doi: 10.1111/j.1600-0773.1984.tb01945.x. PMID 6464782.
- ^ a b Hall H, Ogren SO (1984). "Effects of antidepressant drugs on histamine-H1 receptors in the brain". Life Sci. 34 (6): 597–605. doi: 10.1016/0024-3205(84)90494-6. PMID 6141518.
- ^ a b c d e f Garattini S (1997). "Pharmacology of amineptine, an antidepressant agent acting on the dopaminergic system: a review". Int Clin Psychopharmacol. 12 (Suppl 3): S15–9. doi: 10.1097/00004850-199707003-00003. PMID 9347388. S2CID 23014661.
- ^ Andersen J, Kristensen AS, Bang-Andersen B, Strømgaard K (2009). "Recent advances in the understanding of the interaction of antidepressant drugs with serotonin and norepinephrine transporters". Chem. Commun. (25): 3677–92. doi: 10.1039/b903035m. PMID 19557250.
- ^ "2021 - Placement of Amineptine in Schedule I". Archived from the original on 3 December 2021. Retrieved 30 November 2021.
- ^ "Federal Register". Federal Register. National Archives & Drug Enforcement Administration. 17 November 2022.