| Shigella | |
|---|---|
| |
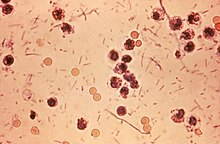
| Photomicrograph of Shigella sp. in a stool specimen | |
|
Scientific classification
| |
| Domain: | Bacteria |
| Phylum: | Pseudomonadota |
| Class: | Gammaproteobacteria |
| Order: | Enterobacterales |
| Family: | Enterobacteriaceae |
| Genus: |
Shigella Castellani & Chalmers 1919 |
| Species | |
Shigella is a genus of bacteria that is Gram-negative, facultatively anaerobic, non–spore-forming, nonmotile, rod-shaped, and is genetically closely related to Escherichia. The genus is named after Kiyoshi Shiga, who discovered it in 1897. [1]
Shigella causes disease in primates, but not in other mammals; it is the causative agent of human shigellosis. [2] It is only naturally found in humans and gorillas. [3] [4] During infection, it typically causes dysentery. [5]
Shigella is a leading cause of bacterial diarrhea worldwide, with 80–165 million annual cases (estimated) [6] and 74,000 to 600,000 deaths. [6] [7] It is one of the top four pathogens that cause moderate-to-severe diarrhea in African and South Asian children. [8]
Classification
Shigella species are classified by three serogroups and one serotype:
- Serogroup A: S. dysenteriae (15 serotypes) [9]
- Serogroup B: S. flexneri (9 serotypes) [10]
- Serogroup C: S. boydii (19 serotypes) [11]
- Serogroup D: S. sonnei (one serotype)[ citation needed]
Groups A–C are physiologically similar; S. sonnei (group D) can be differentiated on the basis of biochemical metabolism assays. [12] Three Shigella groups are the major disease-causing species: S. flexneri is the most frequently isolated species worldwide, and accounts for 60% of cases in the developing world; S. sonnei causes 77% of cases in the developed world, compared to only 15% of cases in the developing world; and S. dysenteriae is usually the cause of epidemics of dysentery, particularly in confined populations such as refugee camps. [13]
Each of the Shigella genomes includes a virulence plasmid that encodes conserved primary virulence determinants. The Shigella chromosomes share most of their genes with those of E. coli K12 strain MG1655. [14]
Phylogenetic studies indicate Shigella is more appropriately treated as a subgroup of Escherichia [15] (see Escherichia coli#Diversity for details).
Pathogenesis
Shigella infection is typically by ingestion. Depending on the host's health, fewer than 100 bacterial cells may cause an infection. [16] Shigella species generally invade the epithelial lining of the colon, causing severe inflammation and death of the cells lining the colon. This inflammation produces the hallmark diarrhea — even dysentery — of Shigella infection. [12] Toxins produced by some strains contribute to disease during infection. S. flexneri strains produce ShET1 and ShET2, which may contribute to diarrhea. [12] S. dysenteriae strains produce the hemolytic Shiga toxin, similar to the verotoxin produced by enterohemorrhagic E. coli. Both Shiga toxin and verotoxin are associated with causing potentially fatal hemolytic-uremic syndrome. [12]
Because they do not interact with the apical surface of epithelial cells — preferring the basolateral side — Shigella species invade the host through the M-cells interspersed in the epithelia of the small intestine. [17] Shigella uses a type-III secretion system that acts as a biological syringe to translocate toxic effector proteins to the target human cell. The effector proteins can alter the metabolism of the target cell — leading, for example, to the lysis of vacuolar membranes or reorganization of actin polymerization to facilitate intracellular motility of Shigella bacteria inside the host cell. For instance, the IcsA effector protein (an autotransporter, not a type-III secretion-system effector) triggers actin reorganization by N-WASP recruitment of Arp2/3 complexes, promoting cell-to-cell spread. [18]
After infection, Shigella cells multiply intracellularly and spread to neighboring epithelial cells, resulting in tissue destruction and the characteristic pathology of shigellosis. [19][ self-published source?] [20] The most common symptoms are diarrhea, fever, nausea, vomiting, stomach cramps, and flatulence. Infection is also commonly known to cause large and painful bowel movements. The stool may contain blood, mucus, or pus. Hence, Shigella cells may cause dysentery. In rare cases, young children may have seizures. Symptoms can take as long as a week to appear, but most often begin two to four days after ingestion. Symptoms usually last for several days, but can last for weeks. Shigella is implicated as one of the pathogenic causes of reactive arthritis worldwide. [21]
Discovery
The Shigella genus is named after Japanese physician Kiyoshi Shiga, who researched the cause of dysentery. Shiga entered the Tokyo Imperial University School of Medicine in 1892, during which he attended a lecture by Shibasaburo Kitasato. Shiga was impressed by Kitasato's intellect and confidence, so after graduating, he went to work for him as a research assistant at the Institute for Infectious Diseases. In 1897, Shiga focused his efforts on what the Japanese referred to as a sekiri (dysentery) outbreak. Such epidemics were detrimental to the Japanese people and occurred often in the late 19th century. The 1897 sekiri epidemic affected >91,000, with a mortality rate of >20%. [22] Shiga studied 32 dysentery patients and used Koch's postulates to successfully isolate and identify the bacterium causing the disease. He continued to study and characterize the bacterium, identified its methods of (Shiga-) toxin production, and worked to create a vaccine for the disease.[ citation needed]
See also
References
- ^ Yabuuchi, Eiko (2002). "Bacillus dysentericus (sic) 1897 was the first taxonomic rather than Bacillus dysenteriae 1898". International Journal of Systematic and Evolutionary Microbiology. 52 (Pt 3): 1041. doi: 10.1099/00207713-52-3-1041. PMID 12054222.
- ^ Ryan, Kenneth James; Ray, C. George, eds. (2004). Sherris medical microbiology: an introduction to infectious diseases (4th ed.). McGraw-Hill Professional Med/Tech. ISBN 978-0-8385-8529-0.[ page needed]
- ^ Pond, Kathy (2005). "Shigella". Water recreation and disease. Plausibility of associated infections: Acute effects, sequelae and mortality. WHO. pp. 113–8. ISBN 978-92-4-156305-5. Archived from the original on June 30, 2013.
- ^ "Shigellosis" (PDF). European Association of Zoo and Wildlife Veterinarians. Archived from the original (PDF) on 2015-09-27.
- ^ Mims, Cedric; Dockrell, Hazel; Goering, Richard; Roitt, Ivan; Wakelin, Derek; Zuckerman, Mark, eds. (2004). Medical Microbiology (3rd ed.). Mosby. p. 287. ISBN 978-0-7234-3259-3.
- ^ a b Bowen A (2016). "Chapter 3: Infectious Diseases Related to Travel". The Yellow Book: Health Information for International Travel. CDC. ISBN 978-0-19-937915-6. Retrieved 22 June 2016.
- ^ Mani, Sachin; Wierzba, Thomas; Walker, Richard I (2016). "Status of vaccine research and development for Shigella". Vaccine. 34 (26): 2887–2894. doi: 10.1016/j.vaccine.2016.02.075. PMID 26979135.
- ^ Kotloff, Karen L; Nataro, James P; Blackwelder, William C; et al. (2013). "Burden and aetiology of diarrhoeal disease in infants and young children in developing countries (the Global Enteric Multicenter Study, GEMS): a prospective, case-control study". The Lancet. 382 (9888): 209–222. doi: 10.1016/S0140-6736(13)60844-2. PMID 23680352. S2CID 205969172.
- ^ Ansaruzzaman, M; Kibriya, AK; Rahman, A; Neogi, PK; Faruque, AS; Rowe, B; Albert, MJ (1995). "Detection of provisional serovars of Shigella dysenteriae and designation as S. dysenteriae serotypes 14 and 15". Journal of Clinical Microbiology. 33 (5): 1423–5. doi: 10.1128/JCM.33.5.1423-1425.1995. PMC 228185. PMID 7615772.
- ^ Knirel, Y. A.; Sun, Q; Senchenkova, SN; Perepelov, AV; Shashkov, AS; Xu, J (2015). "O-Antigen Modifications Providing Antigenic Diversity of Shigella flexneri and Underlying Genetic Mechanisms". Biochemistry (Moscow). 80 (7): 901–914. doi: 10.1134/S0006297915070093. PMID 26542003. S2CID 7360433.
- ^ Yang, Z; Hu, C; Chen, J; Chen, G; Liu, Z (1990). "A new serotype of Shigella boydii". Wei Sheng Wu Xue Bao (in Chinese). 30 (4): 284–95. PMID 2251827.
- ^ a b c d Hale, Thomas L.; Keusch, Gerald T. (1996). "Shigella". In Baron, Samuel (ed.). Medical microbiology (4th ed.). Galveston, Texas: University of Texas Medical Branch. ISBN 978-0-9631172-1-2. PMID 21413292.
- ^ "Shigellosis" (PDF). State of the art of new vaccine research and development. Immunization, Vaccines and Biologicals. World Health Organization. 2006. pp. 10–2. Archived (PDF) from the original on 2015-09-27.
- ^ Yang, Fan; Yang, Jian; Zhang, Xiaobing; Chen, Lihong; Jiang, Yan; Yan, Yongliang; Tang, Xudong; Wang, Jing; Xiong, Zhaohui; Dong, Jie; Xue, Ying; Zhu, Yafang; Xu, Xingye; Sun, Lilian; Chen, Shuxia; Nie, Huan; Peng, Junping; Xu, Jianguo; Wang, Yu; Yuan, Zhenghong; Wen, Yumei; Yao, Zhijian; Shen, Yan; Qiang, Boqin; Hou, Yunde; Yu, Jun; Jin, Qi (2005). "Genome dynamics and diversity of Shigella species, the etiologic agents of bacillary dysentery". Nucleic Acids Research. 33 (19): 6445–58. doi: 10.1093/nar/gki954. PMC 1278947. PMID 16275786.
- ^ Chaudhuri, Roy R.; Henderson, Ian R. (2012-03-01). "The evolution of the Escherichia coli phylogeny". Infection, Genetics and Evolution. 12 (2): 214–226. doi: 10.1016/j.meegid.2012.01.005. ISSN 1567-1348. PMID 22266241.
- ^ Levinson, Warren E (2006). Review of Medical Microbiology and Immunology (9th ed.). McGraw-Hill Medical Publishing Division. p. 30. ISBN 978-0-07-146031-6.
- ^ Mounier, Joëlle; Vasselon, T; Hellio, R; Lesourd, M; Sansonetti, PJ (January 1992). "Shigella flexneri Enters Human Colonic Caco-2 Epithelial Cells through the Basolateral Pole". Infection and Immunity. 60 (1): 237–248. doi: 10.1128/IAI.60.1.237-248.1992. PMC 257528. PMID 1729185.
- ^ Snapper, Scott B.; Takeshima, Fuminao; Antón, Inés; Liu, Ching-Hui; Thomas, Sheila M.; Nguyen, Deanna; Dudley, Darryll; Fraser, Hunter; Purich, Daniel (October 2001). "N-WASP deficiency reveals distinct pathways for cell surface projections and microbial actin-based motility". Nature Cell Biology. 3 (10): 897–904. doi: 10.1038/ncb1001-897. ISSN 1476-4679. PMID 11584271. S2CID 23962367.
- ^ Todar, Kenneth. "Shigella and Shigellosis". Todar's Online Textbook of Bacteriology.[ self-published source]
- ^ Suzuki, Toshihiko; Sasakawa, Chihiro (2001). "Molecular basis of the intracellular spreading of Shigella". Infection and Immunity. 69 (10): 5959–66. doi: 10.1128/IAI.69.10.5959-5966.2001. PMC 98722. PMID 11553531.
- ^ Hill Gaston, J (2003). "Arthritis associated with enteric infection". Best Practice & Research Clinical Rheumatology. 17 (2): 219–39. doi: 10.1016/S1521-6942(02)00104-3. PMID 12787523.
- ^ Trofa, Andrew F.; Ueno-Olsen, Hannah; Oiwa, Ruiko; Yoshikawa, Masanosuke (1999-11-01). "Dr. Kiyoshi Shiga: Discoverer of the Dysentery Bacillus". Clinical Infectious Diseases. 29 (5): 1303–1306. doi: 10.1086/313437. ISSN 1058-4838. PMID 10524979.
External links
- Shigella genomes and related information at PATRIC, a Bioinformatics Resource Center funded by NIAID
- Vaccine Resource Library: Shigellosis and enterotoxigenic Escherichia coli (ETEC)
- US Centers for Disease Control and Prevention. Shigella - Shigellosis