Ներգանգային արյունազեղում (ICH), հայտնի է նաև ուղեղային արյունահոսություն, ներգանգային արյունահոսության տեսակ է որը տեղի է ունենում ուղեղային հյուսվածքում կամ փորոքներում [1]; also known as cerebral bleed, is a type of intracranial bleed that occurs within the brain tissue or ventricles. [1]Ախտանիշները կարող են ներառել գլխացավ, միակողմանի թուլություն, փսխում, ցնցումներ, գիտակցության մթագնում, և պարանոցի կարկամություն [2]։ Symptoms can include headache, one-sided weakness, vomiting, seizures, decreased level of consciousness, and neck stiffness. [2] Հաճախ ախտանիշները ժամանակի հետ վատանում են [3];Often symptoms get worse over time. [3] Fever is also common. [3]Շատ հաճախ արյունահոսությունն առկա է լինում և ուղեղային հյուսվածքում և փորոքներում [3]; In many cases bleeding is present in both the brain tissue and the ventricles. [3]
Պատճառագիտություն և Ախտորոշում
Հիմնական պատճառներն են գլխուղեղի վնասվածք, անևրիզմաներ, զարկերակերակային մալֆորմացիաներ ևգլխուղեղի ուռուցքներ [3]; Causes include brain trauma, aneurysms, arteriovenous malformations, and brain tumors. [3]Սպոնտան արյունահոսությունների ամենամեծ ռիսկի գործոնն են հանդիսանում բարձր զարկերակային ճնշումն ու ամիլոիդոզը [2]; The largest risk factors for spontaneous bleeding are high blood pressure and amyloidosis. [2]Այլ ռիսկի գործոններ են հանդիսանում ալկոհոլիզմը,արյան մեջ ցածր խոլեստերինը, արյան մածուծիկությունն իջեցնող դեղերը և կոկաինի օգտագործումը [2]։Other risk factors include alcoholism, low cholesterol, blood thinners, and cocaine use. [2]Հիմնական ախտորոշիչ մեթոդը համակարգչային շերտագրումն է [3]։ Diagnosis is typically by CT scan. [3]Իշեմիկ կաթվածը այն վիճակներից է, որը դրսևորվում է նույն նշաններով [3]։ Other conditions that may present similarly include ischemic stroke. [3]
Կանխարգելում և բուժում
Բուժումը պետք է իրականացվի ինտենսիվ թերապիայի բաժանմունքում [3]։Treatment should typically be carried out in an intensive care unit. [3]Գայդլայները խորհուրդ են տալիս իջեցնել արյան սիստոլիկ ճնշումը 140մմս․ս․ [3] [4]; Guidelines recommended decreasing the blood pressure to a systolic of 140 mmHg. [3] [4]Հակամակարդիչների ընդունումը հնարավորության դեպքում պետք է դադարեցվի իսկ արյան մեջ գլյուկոզի մակարդակը պետք է պահպանվի նորմայի սահմաններում [3]; Blood thinners should be reversed if possible and blood sugar kept in the normal range. [3]Հիդրոցեֆալիայի բուժման համար կարելի է իրականացնել վիրահատական միջամտություն փորոքային դրենաժի տեղադրմամբ, բայց կորտիկոստերոիդներ բուժման սխեմայում չեն օգտագործվում [3]; Surgery to place a ventricular drain may be used to treat hydrocephalus but corticosteroids should not be used. [3]Որոշ դեպքերում օգտակար են վիրահատական ճանապարհով արյան հեռացումը [3]; Surgery to remov the blood is useful in certain cases. [3]
Համաճարակաբանություն
գլխուղեղային արյունահոսությամբ ամեն տարի տառապում են
Cerebral bleeding affects about 2.5 per 10,000 people each year. [2] It occurs more often in males and older people. [2] About 44% of those affected die within a month. [2] A good outcome occurs in about 20% of those affected. [2] Strokes were first divided into their two major types, bleeding and insufficient blood flow, in 1823. [5]
Signs and symptoms
People with intracerebral bleeding have symptoms that correspond to the functions controlled by the area of the brain that is damaged by the bleed. [6] Other symptoms include those that indicate a rise in intracranial pressure caused by a large mass putting pressure on the brain. [6] Intracerebral bleeds are often misdiagnosed as subarachnoid hemorrhages due to the similarity in symptoms and signs. A severe headache followed by vomiting is one of the more common symptoms of intracerebral hemorrhage. Another common symptom is a patient can collapse. Some people may experience continuous bleeding from the ear. Some patients may also go into a coma before the bleed is noticed.
Causes
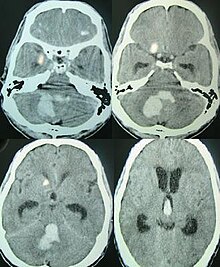
Intracerebral bleeds are the second most common cause of stroke, accounting for 10% of hospital admissions for stroke. [8] High blood pressure raises the risks of spontaneous intracerebral hemorrhage by two to six times. [7] More common in adults than in children, intraparenchymal bleeds are usually due to penetrating head trauma, but can also be due to depressed skull fractures. Acceleration-deceleration trauma, [9] [10] [11] rupture of an aneurysm or arteriovenous malformation (AVM), and bleeding within a tumor are additional causes. Amyloid angiopathy is a not uncommon cause of intracerebral hemorrhage in patients over the age of 55. A very small proportion is due to cerebral venous sinus thrombosis.
ներգանգային արյունազեղման ռիսկի գործոններն են [12]; Risk factors for ICH include: [12]
- Հիպերտենզիա (բարձր զարկերակային ճնշում) Hypertension (high blood pressure)
- Diabetes mellitus
- Menopause
- Cigarette smoking
- Excessive alcohol consumption
- Severe migraine
Traumautic intracerebral hematomas are divided into acute and delayed. Acute intracerebral hematomas occur at the time of the injury while delayed intracerebral hematomas have been reported from as early as 6 hours post injury to as long as several weeks.
Diagnosis

Both computed tomography angiography (CTA) and magnetic resonance angiography (MRA) have been proved to be effective in diagnosing intracranial vascular malformations after ICH. [13] So frequently, a CT angiogram will be performed in order to exclude a secondary cause of hemorrhage [14] or to detect a "spot sign".
Intraparenchymal hemorrhage can be recognized on CT scans because blood appears brighter than other tissue and is separated from the inner table of the skull by brain tissue. The tissue surrounding a bleed is often less dense than the rest of the brain because of edema, and therefore shows up darker on the CT scan. [14]
Location
When due to high blood pressure, intracerebral hemorrhages typically occur in the putamen (50%) or thalamus (15%), cerebrum (10-20%), cerebellum (10-13%), pons (7-15%), or elsewhere in the brainstem (1-6%). [15] [16]
Treatment
Treatment depends substantially on the type of ICH. Rapid CT scan and other diagnostic measures are used to determine proper treatment, which may include both medication and surgery.
- Tracheal intubation is indicated in people with decreased level of consciousness or other risk of airway obstruction. [17]
- IV fluids are given to maintain fluid balance, using isotonic rather than hypotonic fluids. [17]
Medication
- One review found that antihypertensive therapy to bring down the blood pressure in acute phases appears to improve outcomes. [18] Other reviews found an unclear difference between intensive and less intensive blood pressure control. [19] [20] The American Heart Association and American Stroke Association guidelines in 2015 recommended decreasing the blood pressure to a SBP of 140 mmHg. [3] However, the evidence finds tentative usefulness as of 2015. [21]
- Giving Factor VIIa within 4 hours limits the bleeding and formation of a hematoma. However, it also increases the risk of thromboembolism. [17] It thus overall does not result in better outcomes in those without hemophilia. [22]
- Frozen plasma, vitamin K, protamine, or platelet transfusions may be given in case of a coagulopathy. [17] Platelets however appear to worsen outcomes in those with spontaneous intracerebral bleeding on antiplatelet medication. [23]
- Fosphenytoin or other anticonvulsant is given in case of seizures or lobar hemorrhage. [17]
- H2 antagonists or proton pump inhibitors are commonly given for to try to prevent stress ulcers, a condition linked with ICH. [17]
- Corticosteroids, were thought to reduce swelling. However, in large controlled studies, corticosteroids have been found to increase mortality rates and are no longer recommended. [24] [25]
Surgery
Surgery is required if the hematoma is greater than 3 cm (1 in), if there is a structural vascular lesion or lobar hemorrhage in a young patient. [17]
- A catheter may be passed into the brain vasculature to close off or dilate blood vessels, avoiding invasive surgical procedures. [26]
- Aspiration by stereotactic surgery or endoscopic drainage may be used in basal ganglia hemorrhages, although successful reports are limited. [17]
- A craniectomy may take place, where part of the skull is removed to allow a swelling brain room to expand without being squeezed.
Prognosis
The risk of death from an intraparenchymal bleed in traumatic brain injury is especially high when the injury occurs in the brain stem. [27] Intraparenchymal bleeds within the medulla oblongata are almost always fatal, because they cause damage to cranial nerve X, the vagus nerve, which plays an important role in blood circulation and breathing. [9] This kind of hemorrhage can also occur in the cortex or subcortical areas, usually in the frontal or temporal lobes when due to head injury, and sometimes in the cerebellum. [9] [28]
For spontaneous ICH seen on CT scan, the death rate ( mortality) is 34–50% by 30 days after the insult, [7] and half of the deaths occur in the first 2 days. [29] Even though the majority of deaths occurs in the first days after ICH, survivors have a long term excess mortality of 27% compared to the general population. [30]
Epidemiology
It accounts for 20% of all cases of cerebrovascular disease in the United States, behind cerebral thrombosis (40%) and cerebral embolism (30%). [31]
Research
The inflammatory response triggered by stroke has been viewed as harmful in the early stage, focusing on blood-borne leukocytes, neutrophils and macrophages, and resident microglia and astrocytes. [32] A human postmortem study shows that inflammation occurs early and persists for several days after ICH. [33] Modulating microglial activation and polarization might mitigate intracerebral hemorrhage-induced brain injury and improve brain repair. [34] A new area of interest is the role of mast cells in ICH. [35]
References
- ^ a b Naidich, Thomas P.; Castillo, Mauricio; Cha, Soonmee; Smirniotopoulos, James G. (2012). Imaging of the Brain, Expert Radiology Series,1: Imaging of the Brain. Elsevier Health Sciences. p. 387. ISBN 978-1416050094. Archived from the original on 2016-10-02.
- ^ a b c d e f g h i j Caceres, JA; Goldstein, JN (August 2012). "Intracranial hemorrhage". Emergency Medicine Clinics of North America. 30 (3): 771–94. doi: 10.1016/j.emc.2012.06.003. PMC 3443867. PMID 22974648.
- ^
a
b
c
d
e
f
g
h
i
j
k
l
m
n
o
p
q
r
s
t
u
v Hemphill JC, 3rd; Greenberg, SM; Anderson, CS; Becker, K; Bendok, BR; Cushman, M; Fung, GL; Goldstein, JN; Macdonald, RL; Mitchell, PH; Scott, PA; Selim, MH; Woo, D; American Heart Association Stroke, Council; Council on Cardiovascular and Stroke, Nursing; Council on Clinical, Cardiology (July 2015).
"Guidelines for the Management of Spontaneous Intracerebral Hemorrhage: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association". Stroke: A Journal of Cerebral Circulation. 46 (7): 2032–60.
doi:
10.1161/str.0000000000000069.
PMC
4462131.
PMID
26022637.
{{ cite journal}}: CS1 maint: numeric names: authors list ( link) - ^ a b Ko, SB; Yoon, BW (December 2017). "Blood Pressure Management for Acute Ischemic and Hemorrhagic Stroke: The Evidence". Seminars in Respiratory and Critical Care Medicine. 38 (6): 718–725. doi: 10.1055/s-0037-1608777. PMID 29262429. S2CID 19970695.
- ^ Hennerici, Michael (2003). Imaging in Stroke. Remedica. p. 1. ISBN 9781901346251. Archived from the original on 2016-10-02.
- ^ a b Vinas FC and Pilitsis J. 2006. "Penetrating Head Trauma." Archived 2005-09-13 at the Wayback Machine Emedicine.com.
- ^
a
b
c
d Yadav YR, Mukerji G, Shenoy R, Basoor A, Jain G, Nelson A (2007).
"Endoscopic management of hypertensive intraventricular haemorrhage with obstructive hydrocephalus". BMC Neurol. 7: 1.
doi:
10.1186/1471-2377-7-1.
PMC
1780056.
PMID
17204141.
{{ cite journal}}: CS1 maint: unflagged free DOI ( link) - ^ Go AS, Mozaffarian D, Roger VL, et al. (January 2013). "Heart disease and stroke statistics--2013 update: a report from the American Heart Association". Circulation. 127 (1): e6–e245. doi: 10.1161/CIR.0b013e31828124ad. PMC 5408511. PMID 23239837.
- ^ a b c McCaffrey P. 2001. "The Neuroscience on the Web Series: CMSD 336 Neuropathologies of Language and Cognition." Archived 2005-11-25 at the Wayback Machine California State University, Chico. Retrieved on June 19, 2007.
- ^ Orlando Regional Healthcare, Education and Development. 2004. "Overview of Adult Traumatic Brain Injuries." Archived 2008-02-27 at the Wayback Machine Retrieved on 2008-01-16.
- ^ Shepherd S. 2004. "Head Trauma." Archived 2005-10-26 at the Wayback Machine Emedicine.com. Retrieved on June 19, 2007.
- ^ a b Feldmann, Edward; Broderick, Joseph P.; Kernan, Walter N.; Viscoli, Catherine M.; Brass, Lawrence M.; Brott, Thomas; Morgenstern, Lewis B.; Lee Wilterdink, Janet; Horwitz, Ralph I. (2005). "Major Risk Factors for Intracerebral Hamorrhage in the Young Are Modifiable". Stroke. 36 (9): 1881–5. doi: 10.1161/01.str.0000177480.62341.6b. PMID 16081867. S2CID 6310754. Archived from the original on 2009-03-05.
-
^ Josephson, Colin B; White, Philip M; Krishan, Ashma; Al-Shahi Salman, Rustum (1 September 2014).
"Computed tomography angiography or magnetic resonance angiography for detection of intracranial vascular malformations in patients with intracerebral haemorrhage". The Cochrane Library. 9 (9): CD009372.
doi:
10.1002/14651858.CD009372.pub2.
PMC
6544803.
PMID
25177839.
{{ cite journal}}: CS1 maint: url-status ( link) - ^ a b Yeung R, Ahmad T, Aviv RI, Noel de Tilly L, Fox AJ, Symons SP (2009). "Comparison of CTA to DSA in determining the etiology of spontaneous ICH". Canadian Journal of Neurological Sciences. 36 (2): 176–180. doi: 10.1017/s0317167100006533. PMID 19378710. S2CID 26818365.
- ^ Greenberg, Mark S. (2016). Handbook of Neurosurgery. ISBN 9781626232419.
- ^ Prayson, Richard A. (2012). Neuropathology. Elsevier Health Sciences. p. 49. ISBN 978-1437709490. Archived from the original on 2017-03-12.
- ^ a b c d e f g h eMedicine Specialties > Neurology > Neurological Emergencies > Intracranial Haemorrhage: Treatment & Medication. Archived 2009-03-12 at the Wayback Machine By David S Liebeskind, MD. Updated: Aug 7, 2006
- ^ Tsivgoulis, G; Katsanos, AH; Butcher, KS; Boviatsis, E; Triantafyllou, N; Rizos, I; Alexandrov, AV (21 October 2014). "Intensive blood pressure reduction in acute intracerebral hemorrhage: A meta-analysis". Neurology. 83 (17): 1523–9. doi: 10.1212/wnl.0000000000000917. PMID 25239836. S2CID 36315871.
-
^ Ma, J; Li, H; Liu, Y; You, C; Huang, S; Ma, L (2015). "Effects of Intensive Blood Pressure Lowering on Intracerebral Hemorrhage Outcomes: A Meta-Analysis of Randomized Controlled Trials". Turkish Neurosurgery. 25 (4): 544–51.
doi:
10.5137/1019-5149.JTN.9270-13.0 (inactive 2022-06-11).
PMID
26242330.
{{ cite journal}}: CS1 maint: DOI inactive as of June 2022 ( link) - ^ Boulouis, Gregoire; Morotti, Andrea; Goldstein, Joshua N.; Charidimou, Andreas (1 April 2017). "Intensive blood pressure lowering in patients with acute intracerebral haemorrhage: clinical outcomes and haemorrhage expansion. Systematic review and meta-analysis of randomised trials". Journal of Neurology, Neurosurgery, and Psychiatry. 88 (4): 339–345. doi: 10.1136/jnnp-2016-315346. ISSN 1468-330X. PMID 28214798. S2CID 25397701.
-
^ Ma, J; Li, H; Liu, Y; You, C; Huang, S; Ma, L (2015). "Effects of Intensive Blood Pressure Lowering on Intracerebral Hemorrhage Outcomes: A Meta-Analysis of Randomized Controlled Trials". Turkish Neurosurgery. 25 (4): 544–51.
doi:
10.5137/1019-5149.JTN.9270-13.0 (inactive 2022-06-11).
PMID
26242330.
{{ cite journal}}: CS1 maint: DOI inactive as of June 2022 ( link) - ^ Yuan, ZH; Jiang, JK; Huang, WD; Pan, J; Zhu, JY; Wang, JZ (June 2010). "A meta-analysis of the efficacy and safety of recombinant activated factor VII for patients with acute intracerebral hemorrhage without hemophilia". Journal of Clinical Neuroscience. 17 (6): 685–93. doi: 10.1016/j.jocn.2009.11.020. PMID 20399668. S2CID 30590573.
- ^ Al-Shahi Salman, R; Law, ZK; Bath, PM; Steiner, T; Sprigg, N (17 April 2018). "Haemostatic therapies for acute spontaneous intracerebral haemorrhage". The Cochrane Database of Systematic Reviews. 2018 (4): CD005951. doi: 10.1002/14651858.CD005951.pub4. PMC 6494564. PMID 29664991.
- ^ Roberts, Ian; Yates, David; Sandercock, Peter; Farrell, Barbara; Wasserberg, Jonathan (9 October 2016). "Effect of intravenous corticosteroids on death within 14 days in 10008 adults with clinically significant head injury (MRC CRASH trial): randomised placebo-controlled trial". Lancet. 364 (9442): 1321–1328. doi: 10.1016/S0140-6736(04)17188-2. ISSN 1474-547X. PMID 15474134. S2CID 30210176.
-
^ Edwards, P; Arango, M; Balica, L; Cottingham, R; El-Sayed, H (undefined NaN). "Final results of MRC CRASH, a randomised placebo-controlled trial of intravenous corticosteroid in adults with head injury-outcomes at 6 months". Lancet. 365 (9475): 1957–9.
doi:
10.1016/s0140-6736(05)66552-x.
PMID
15936423.
S2CID
27713031.
{{ cite journal}}: Check date values in:|date=( help) - ^ Cedars-Sinai Health System - Cerebral Hemorrhages Archived 2009-03-12 at the Wayback Machine Retrieved on 02/25/2009
- ^ Sanders MJ and McKenna K. 2001. Mosby's Paramedic Textbook, 2nd revised Ed. Chapter 22, "Head and Facial Trauma." Mosby.
- ^ Graham DI and Gennareli TA. Chapter 5, "Pathology of Brain Damage After Head Injury" Cooper P and Golfinos G. 2000. Head Injury, 4th Ed. Morgan Hill, New York.
- ^ Broderick, J.; Connolly, S.; Feldmann, E.; Hanley, D.; Kase, C.; Krieger, D.; Mayberg, M.; Morgenstern, L.; Ogilvy, C. S.; Vespa, P.; Zuccarello, M. (3 May 2007). "Guidelines for the Management of Spontaneous Intracerebral Hemorrhage in Adults: 2007 Update: A Guideline From the American Heart Association/American Stroke Association Stroke Council, High Blood Pressure Research Council, and the Quality of Care and Outcomes in Research Interdisciplinary Working Group: The American Academy of Neurology affirms the value of this guideline as an educational tool for neurologists". Stroke. 38 (6): 2001–2023. doi: 10.1161/strokeaha.107.183689. PMID 17478736. S2CID 1545807.
- ^ Hansen, B.M.; Nilsson O.G.; Anderson H; et al. (Oct 2013). "Long term (13 years) prognosis after primary intracerebral haemorrhage: a prospective population based study of long term mortality, prognostic factors and causes of death". Journal of Neurology, Neurosurgery & Psychiatry. 84 (10): 1150–1155. doi: 10.1136/jnnp-2013-305200. PMID 23715913. S2CID 40379279. Archived from the original on 2014-02-22.
- ^ Page 117 in: Henry S. Schutta; Lechtenberg, Richard (1998). Neurology practice guidelines. New York: M. Dekker. ISBN 978-0-8247-0104-8.
- ^ Wang J (December 2010). "Preclinical and clinical research on inflammation after intracerebral hemorrhage". Prog. Neurobiol. 92 (4): 463–77. doi: 10.1016/j.pneurobio.2010.08.001. PMC 2991407. PMID 20713126.
- ^ Wu H, Zhang Z, Hu X, Zhao R, Song Y, Ban X, Qi J, Wang J (2010). "Dynamic changes of inflammatory markers in brain after hemorrhagic stroke in humans: a postmortem study". Brain Research. 1342 (1342): 111–1117. doi: 10.1016/j.brainres.2010.04.033. PMC 2885522. PMID 20420814.
- ^ Lan X, Han X, Li Q, Yang QW, Wang J (2017). "Modulators of microglial activation and polarization after intracerebral haemorrhage". Nat Rev Neurol. 13 (7): 420–433. doi: 10.1038/nrneurol.2017.69. PMC 5575938. PMID 28524175.
- ^ Johannes Lindsberg, Perttu; Strbian, Daniel; Karjalainen-Lindsberg, Marja-Liisa (2010). "Mast Cells as Early Responders in the Regulation of Acute Blood–Brain Barrier Changes after Cerebral Ischemia and Hemorrhage". Journal of Cerebral Blood Flow & Metabolism. 30 (4): 689–702. doi: 10.1038/jcbfm.2009.282. PMC 2949160. PMID 20087366.
Further reading
- Hemphill JC, 3rd; Greenberg, SM; Anderson, CS; Becker, K; Bendok, BR; Cushman, M; Fung, GL; Goldstein, JN; Macdonald, RL; Mitchell, PH; Scott, PA; Selim, MH; Woo, D (28 May 2015).
"Guidelines for the Management of Spontaneous Intracerebral Hemorrhage: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association". Stroke: A Journal of Cerebral Circulation. 46 (7): 2032–60.
doi:
10.1161/STR.0000000000000069.
PMC
4462131.
PMID
26022637.
{{ cite journal}}: CS1 maint: numeric names: authors list ( link)
External links
Category:Cerebrovascular diseases
Category:Neurotrauma
Category:Stroke
Category:Wikipedia medicine articles ready to translate
Category:RTTNEURO