
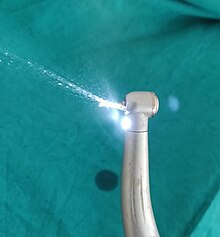
A dental aerosol is an aerosol that is produced from dental instrument, dental handpieces, three-way syringes, and other high-speed instruments. These aerosols may remain suspended in the clinical environment. [1] Dental aerosols can pose risks to the clinician, staff, and other patients. The heavier particles (e.g., >50 µm) contained within the aerosols are likely to remain suspended in the air for relatively short period and settle quickly onto surfaces, however, the lighter particles may remain suspended for longer periods and may travel some distance from the source. [2] These smaller particles are capable of becoming deposited in the lungs when inhaled and provide a route of diseases transmission. [3] Different dental instruments produce varying quantities of aerosol, and therefore are likely to pose differing risks of dispersing microbes from the mouth. Air turbine dental handpieces generally produce more aerosol, with electric micromotor handpieces producing less, although this depends on the configuration of water coolant used by the handpiece. [4] [5]
Composition
These dental aerosols are bioaerosols which may be contaminated with bacteria, fungi, and viruses from the oral cavity, skin, and the water used in dental units. [6] Dental aerosols also have micro-particles from dental burs, and silica particles which are one of the components of dental filling materials like dental composite. [7] Depending upon the procedure and site, the aerosol composition may change from patient to patient. Apart from microorganisms, these aerosols may consist of particles from saliva, gingival crevicular fluid, blood, dental plaque, calculus, tooth debris, oronasal secretions, oil from dental handpieces, and micro-particles from grinding of the teeth and dental materials. [8] They may also consist of abrasive particles that are expelled during air abrasion and polishing methods. [3]
Size
Dental aerosols contain a wide range of particles with the majority being less than 50 µm. The smaller particles with size between 0.5 and 10 µm are more likely to be inhaled and have the potential to transmit infection. [3] Smaller particles are likely to remain suspended for longer periods of time, and may travel further from the source. Settling time of particles is described by Stokes' law in part as a function of their aerodynamic diameter.
Potential hazards and mitigation
The water used in the dental units may be contaminated with Legionella, and the aerosols produced by dental handpieces may contribute to the spread of the Legionella in the environment; there is therefore a risk of inhalation by the dentist, staff and patients. [9] The dental unit water lines (DUWLs) may also be contaminated with other bacteria like Mycobacterium spp and Pseudomonas aeruginosa. [10] Infection from Legionella species causes infections like Legionellosis and several pneumonia like diseases. [11] However, still there is no strong evidence that suggests the dentists are at greater occupational risk from Legionella. [9] Transmission of tuberculosis also occurs from the cough producing procedures on the patients with tuberculosis that involve production of aerosols. [12] Mycobacterium tuberculosis is transmitted in the form of droplet nuclei which are smaller than 5 µm which stay suspended in the environment for longer duration. The development of active tuberculosis in Dental Health Care Workers (DHCWs) is less likely than the rest of the other Health Care Workers (HCWs). There are lacking evidences to prove the active tuberculosis development resulting from this transmission in Dental health care Workers (DHCWs). [13]
The virus that caused the COVID-19 pandemic is named as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) by the International Committee on Taxonomy of Viruses (ICTV) on 11 February 2020. [14] SARS-CoV-2 remains stable in aerosols for several hours. [15] The virus is viable for hours in aerosols and for few days on surfaces, hence the transmission of SARS-CoV-2 is feasible through aerosols and also shows fomite transmission. [16]
Dentists have previously been described as one of the top of the working groups with high risk of exposure to SARS-CoV-2. Due to the close proximity of the dental health care workers to the patients, dental procedures involving aerosol production is not advisable in patients who tested positive for COVID-19 except for emergency dental treatment. [17] On 16 March 2020, the American Dental Association ( ADA) has advised dentists to postpone all elective procedures. [18] ADA also developed guidance specific to address dental services during the COVID-19 pandemic. [19]
Elements like calcium, aluminium, silica and phosphorus can also be found in the dental aerosols produced during the procedures like debonding of orthodontic appliances. [20] These particles may range from 2 to 30 µm in diameter and there are chances of inhaling them. [21]
A number of methods have been proposed, and are widely used, to control dental aerosols and reduce risk of disease transmission. For example, dental aerosols can be controlled or reduced using dental suction, [22] rubber dam, [5] alternative handpieces, [2] and local exhaust ventilation (extra-oral suction). [23]
See also
References
- ^ Chuang CY, Cheng HC, Yang S, Fang W, Hung PC, Chuang SY (2014). "Investigation of the spreading characteristics of bacterial aerosol contamination during dental scaling treatment". Journal of Dental Sciences. 9 (3): 294–296. doi: 10.1016/j.jds.2014.06.002.
- ^ a b Holliday R, Allison JR, Currie CC, Edwards DC, Bowes C, Pickering K, et al. (February 2021). "Evaluating contaminated dental aerosol and splatter in an open plan clinic environment: Implications for the COVID-19 pandemic". Journal of Dentistry. 105: 103565. doi: 10.1016/j.jdent.2020.103565. PMC 7787509. PMID 33359041.
- ^ a b c Harrel SK, Molinari J (April 2004). "Aerosols and splatter in dentistry: a brief review of the literature and infection control implications". Journal of the American Dental Association. 135 (4): 429–37. doi: 10.14219/jada.archive.2004.0207. PMC 7093851. PMID 15127864.
- ^ Allison JR, Edwards DC, Bowes C, Pickering K, Dowson C, Stone SJ, et al. (September 2021). "The effect of high-speed dental handpiece coolant delivery and design on aerosol and droplet production". Journal of Dentistry. 112: 103746. doi: 10.1016/j.jdent.2021.103746. PMID 34265364. S2CID 235961737.
- ^ a b Vernon JJ, Black EV, Dennis T, Devine DA, Fletcher L, Wood DJ, Nattress BR (August 2021). "Dental Mitigation Strategies to Reduce Aerosolization of SARS-CoV-2". Journal of Dental Research. 100 (13): 1461–1467. doi: 10.1177/00220345211032885. PMC 8649409. PMID 34338580. S2CID 236775223.
- ^ Zemouri C, de Soet H, Crielaard W, Laheij A (2017-05-22). Zhou D (ed.). "A scoping review on bio-aerosols in healthcare and the dental environment". PLOS ONE. 12 (5): e0178007. Bibcode: 2017PLoSO..1278007Z. doi: 10.1371/journal.pone.0178007. PMC 5439730. PMID 28531183.
- ^ Sivakumar I, Arunachalam KS, Solomon E (November 2012). "Occupational health hazards in a prosthodontic practice: review of risk factors and management strategies". The Journal of Advanced Prosthodontics. 4 (4): 259–65. doi: 10.4047/jap.2012.4.4.259. PMC 3517967. PMID 23236581.
- ^ King TB, Muzzin KB, Berry CW, Anders LM (January 1997). "The effectiveness of an aerosol reduction device for ultrasonic scalers". Journal of Periodontology. 68 (1): 45–9. doi: 10.1902/jop.1997.68.1.45. PMID 9029451.
- ^ a b Petti S, Vitali M (July 2017). "Occupational risk for Legionella infection among dental healthcare workers: meta-analysis in occupational epidemiology". BMJ Open. 7 (7): e015374. doi: 10.1136/bmjopen-2016-015374. PMC 5734417. PMID 28710211.
- ^ "WHO | Water safety in buildings". WHO. Archived from the original on September 30, 2016. Retrieved 2020-03-13.
- ^ Legionella and the prevention of legionellosis. World Health Organization. 2007.
- ^ "Guidelines for Preventing the Transmission of Mycobacterium tuberculosis in Health-Care Settings, 2005". www.cdc.gov. Retrieved 2020-03-16.
- ^ Petti S (June 2016). "Tuberculosis: Occupational risk among dental healthcare workers and risk for infection among dental patients. A meta-narrative review". Journal of Dentistry. 49: 1–8. doi: 10.1016/j.jdent.2016.04.003. PMID 27106547.
- ^ "Naming the coronavirus disease (COVID-19) and the virus that causes it". www.who.int. Retrieved 2020-03-19.
- ^ "New coronavirus stable for hours on surfaces". National Institutes of Health (NIH). 2020-03-17. Retrieved 2020-03-19.
- ^ van Doremalen N, Bushmaker T, Morris DH, Holbrook MG, Gamble A, Williamson BN, et al. (April 2020). "Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1". The New England Journal of Medicine (letter). 382 (16): 1564–1567. doi: 10.1056/nejmc2004973. PMC 7121658. PMID 32182409.
- ^ Gamio L (2020-03-15). "The Workers Who Face the Greatest Coronavirus Risk". The New York Times. ISSN 0362-4331. Retrieved 2020-03-16.
- ^ "ADA Calls Upon Dentists to Postpone Elective Procedures". American Dental Association. 16 March 2020. Archived from the original on 8 May 2021. Retrieved 23 March 2020.
- ^ "COVID-19 Resources for Dentists". American Dental Association. Retrieved 23 March 2020.
- ^ Day CJ, Price R, Sandy JR, Ireland AJ (January 2008). "Inhalation of aerosols produced during the removal of fixed orthodontic appliances: a comparison of 4 enamel cleanup methods". American Journal of Orthodontics and Dentofacial Orthopedics. 133 (1): 11–7. doi: 10.1016/j.ajodo.2006.01.049. PMID 18174065.
- ^ Ireland AJ, Moreno T, Price R (December 2003). "Airborne particles produced during enamel cleanup after removal of orthodontic appliances". American Journal of Orthodontics and Dentofacial Orthopedics. 124 (6): 683–6. doi: 10.1016/s0889-5406(03)00623-1. PMID 14666082.
- ^ Allison JR, Currie CC, Edwards DC, Bowes C, Coulter J, Pickering K, et al. (January 2021). "Evaluating aerosol and splatter following dental procedures: Addressing new challenges for oral health care and rehabilitation". Journal of Oral Rehabilitation. 48 (1): 61–72. doi: 10.1111/joor.13098. PMC 7537197. PMID 32966633.
- ^ Allison JR, Dowson C, Pickering K, Červinskytė G, Durham J, Jakubovics NS, Holliday R (November 2021). "Local Exhaust Ventilation to Control Dental Aerosols and Droplets". Journal of Dental Research. 101 (4): 384–391. doi: 10.1177/00220345211056287. PMC 8935467. PMID 34757884. S2CID 243987221.
Further reading
- Shirazi S, Stanford CM, Cooper LF (March 2021). "Characteristics and Detection Rate of SARS-CoV-2 in Alternative Sites and Specimens Pertaining to Dental Practice: An Evidence Summary". Journal of Clinical Medicine. 10 (6): 1158. doi: 10.3390/jcm10061158. PMC 8000787. PMID 33802043.
- Shirazi S, Stanford CM, Cooper LF (May 2021). "Testing for COVID-19 in dental offices: mechanism of action, application and interpretation of laboratory and point-of-care screening tests". The Journal of the American Dental Association. 152 (7): 514–525.e8. doi: 10.1016/j.adaj.2021.04.019. ISSN 0002-8177. PMC 8096195. PMID 34176567.
External links
- "Coronavirus Resource Center for Dentists". American Dental Association (ADA). Archived from the original on 2020-03-18. Retrieved 2020-03-18.