| Mpox in the Democratic Republic of the Congo | |
|---|---|
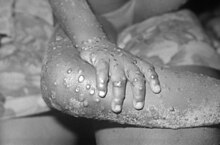
 Mpox (large lymph node in neck), DRC 1996/1997 | |
| Disease | Mpox |
| Virus strain | Monkeypox virus |
| Source | Initially mainly animal contact in rainforest, later greater human-to-human transmission |
| Location | Democratic Republic of the Congo |
Mpox is endemic in western and central Africa, with the majority of cases occurring in the Democratic Republic of the Congo (DRC), where the disease is reportable. [1] [2] There, the more virulent Congo basin virus type has been affecting some of the world's poorest and socially excluded communities. [3]
Many cases occur sporadically or in small clusters, but large outbreaks also occur. [2]
Early cases
The world's first case of human mpox was detected in a nine-month old child in 1970 in the Democratic Republic of the Congo (then Zaire), [4] [5] two years after it reported its last case of smallpox. [6] The onset of their rash was on 24 August. [7] That year, the disease was identified in another four children, including three in Liberia who were playmates. [8] At the time, evidence of the virus was found in non-human primates in Liberia and Sierre Leone. [8]
Active surveillance by the World Health Organization (WHO) between 1981 and 1986, identified 338 cases with a human-to-human transmission rate of 28%. [9] [10] Until 1986, 95% of cases worldwide were identified in the DRC. [11] Cases were rare in people over the age of 15-years, and over two-thirds of infections could be traced to animal contact within the rainforests. [12] Initially it was uncommon for a family member to contract the infection unless they did not have a smallpox scar. [12]
1996 reemergence
A reemergence of the disease in the DRC in 1996 also saw a large number of reported but not all laboratory confirmed cases, with a high transmission rate and lower fatality rate; leading experts to believe a significant number may have actually been chicken pox. [10] [13] Some likely had both mpox and chickenpox at the same time. [6] The DRC's Kasaï-Oriental region saw the largest number of cases during 1996–1997. [6]
Between 1996 and 2005, mpox cases appeared increasingly in gradually older people, with less than a quarter of cases being traced to rainforest animal contact, and with greater close contact infections. [12] Between January 2001 and December 2004, 2,734 cases of suspected human mpox were reported from the DRC. [10] However, civil war limited surveillance and only 171 clinical specimens were obtained from 136 suspected cases; less than 5% of all reported cases. [10]
-
Mpox outbreak in DRC (1997)
-
The US epidemiologic team after having landed at Lodja Airport - Zaire 1997
-
Testing of Gambian rats (1997)
-
Educational meeting DRC (1997)
2005 onwards
After 2005, the DRC was reporting more than 1000 suspected cases per year. [14] Between November 2005 and November 2007, 760 laboratory-confirmed human mpox cases were detected; particularly in people living in forested areas, males, age less than 15-years, and no previous smallpox vaccination. [15]
Many cases occur sporadically or in small clusters, but large outbreaks also occur. [2] The risk of human-to-human transmission within households in the DRC was noted to range from 50% to 100% during the 2013 outbreak. [6] The DRC's Bokungu Health Zone saw an increase in cases of 600-fold that year. [2] In 2019 the DRC reported 3,794 suspected cases and 73 deaths. [11] In the first nine-months of 2020, it reported over 4,500 suspected cases of mpox, including 171 deaths. [11]
Mpox is reportable in the DRC, where the disease is endemic, and disease burden remains high. [2] [16] There, the more virulent Congo basin virus type has been affecting some of the world's poorest and socially excluded communities. [3] A regional surveillance system collects reports of all suspected mpox cases, and where possible, they may be investigated. [2]
2023-2024 outbreak
During 2023, a Clade I outbreak of mpox disease in the DRC resulted in 14,626 suspected cases being reported, with 654 associated deaths, making for a case-fatality rate (CFR) of 4.5%. The outbreak continued into 2024 with an additional 3,576 suspected mpox cases and 265 deaths being reported in the DRC through the first 9 weeks of the year, making for an estimated CFR of 7.4%. [17]
The outbreak appears to be of a primarily sexually transmitted nature and cases are occurring in areas without a history of mpox, such as South Kivu and Kinshasa. The outbreak seems to consist of two separate sub-variants of clade I, with one of the sub-variants having a novel mutation making detection with standard assays unreliable. [17]
The outbreak spread to the neighbouring country of the Republic of Congo, with 43 mpox cases being reported in March 2024. [17]
References
- ^ "Multi-country monkeypox outbreak: situation update". www.who.int. World Health Organization. 4 June 2022. Retrieved 11 June 2022.
- ^ a b c d e f Nolen LD, Osadebe L, Katomba J, Likofata J, Mukadi D, Monroe B, Doty J, Hughes CM, Kabamba J, Malekani J, Bomponda PL, Lokota JI, Balilo MP, Likafi T, Lushima RS, Ilunga BK, Nkawa F, Pukuta E, Karhemere S, Tamfum JJ, Nguete B, Wemakoy EO, McCollum AM, Reynolds MG (June 2016). "Extended Human-to-Human Transmission during a Monkeypox Outbreak in the Democratic Republic of the Congo". Emerging Infectious Diseases. 22 (6): 1014–21. doi: 10.3201/eid2206.150579. PMC 4880088. PMID 27191380.
- ^ a b Adler H, Gould S, Hine P, Snell LB, Wong W, Houlihan CF, Osborne JC, Rampling T, Beadsworth MB, Duncan CJ, Dunning J, Fletcher TE, Hunter ER, Jacobs M, Khoo SH, Newsholme W, Porter D, Porter RJ, Ratcliffe L, Schmid ML, Semple MG, Tunbridge AJ, Wingfield T, Price NM (24 May 2022). "Clinical features and management of human monkeypox: a retrospective observational study in the UK". The Lancet. Infectious Diseases. 22 (8): S1473–3099(22)00228–6. doi: 10.1016/S1473-3099(22)00228-6. ISSN 1474-4457. PMC 9300470. PMID 35623380. S2CID 249057804.
- ^ Fenner F, Wittek R, Dumbell KR (1988). "8. Monkeypox virus". The Orthopoxviruses. Elsevier. pp. 227–267. ISBN 978-0-323-15022-4.
- ^ Fenner F, santé Om, Organization WH, Henderson DA, Arita I, Jezek Z, Ladnyi ID (1988). "29. Human monkeypox and other poxvirus infections of man". Smallpox and Its Eradication (PDF). World Health Organization. pp. 1287–1319. ISBN 978-92-4-156110-5.
- ^ a b c d Sutcliffe CG, Rimone AW, Moss WJ (2020). "32.2. Poxviruses". In Ryan ET, Hill DR, Solomon T, Aronson N, Endy TP (eds.). Hunter's Tropical Medicine and Emerging Infectious Diseases E-Book (Tenth ed.). Edinburgh: Elsevier. pp. 272–277. ISBN 978-0-323-55512-8.
- ^ Arita I, Henderson DA (1976). "Monkeypox and whitepox viruses in West and Central Africa". Bulletin of the World Health Organization. 53 (4): 347–53. PMC 2366520. PMID 186209.
- ^ a b Cho CT, Wenner HA (March 1973). "Monkeypox virus". Bacteriological Reviews. 37 (1): 1–18. doi: 10.1128/br.37.1.1-18.1973. ISSN 0005-3678. PMC 413801. PMID 4349404.
- ^ Essbauer S, Meyer H (2007). "Genus Orthopoxvirus: Monkeypox virus". In Mercer A, Schmidt A, Weber O (eds.). Poxviruses. Springer. p. 66. ISBN 978-3-7643-7556-0.
- ^ a b c d Rimoin AW, Kisalu N, Kebela-Ilunga B, Mukaba T, Wright LL, Formenty P, Wolfe ND, Shongo RL, Tshioko F, Okitolonda E, Muyembe JJ, Ryder R, Meyer H (June 2007). "Endemic human monkeypox, Democratic Republic of Congo, 2001-2004". Emerging Infectious Diseases. 13 (6): 934–7. doi: 10.3201/eid1306.061540. PMC 2792850. PMID 17553242.
- ^ a b c "Monkeypox – Democratic Republic of the Congo". www.who.int. World Health Organization. Archived from the original on 5 June 2022. Retrieved 5 June 2022.
- ^ a b c Hobson G, Adamson J, Adler H, Firth R, Gould S, Houlihan C, Johnson C, Porter D, Rampling T, Ratcliffe L, Russell K, Shankar AG, Wingfield T (August 2021). "Family cluster of three cases of monkeypox imported from Nigeria to the United Kingdom, May 2021". Euro Surveillance. 26 (32). doi: 10.2807/1560-7917.ES.2021.26.32.2100745. ISSN 1560-7917. PMC 8365177. PMID 34387184.
- ^ Breman JG, Kalisa R, Steniowski MV, Zanotto E, Gromyko AI, Arita I (1980). "Human monkeypox, 1970-79". Bull World Health Organ. 58 (2): 165–182. PMC 2395797. PMID 6249508.
- ^ Sklenovská N (2020). "2. Monkeypox". In Malik YS, Singh RK, Dhama K (eds.). Animal-Origin Viral Zoonoses. Singapore: Springer. pp. 39–68. ISBN 978-981-15-2650-3.
- ^ Rimoin AW, Mulembakani PM, Johnston SC, Lloyd Smith JO, Kisalu NK, Kinkela TL, Blumberg S, Thomassen HA, Pike BL, Fair JN, Wolfe ND, Shongo RL, Graham BS, Formenty P, Okitolonda E, Hensley LE, Meyer H, Wright LL, Muyembe JJ (14 September 2010). "Major increase in human monkeypox incidence 30 years after smallpox vaccination campaigns cease in the Democratic Republic of Congo". Proceedings of the National Academy of Sciences of the United States of America. 107 (37): 16262–16267. Bibcode: 2010PNAS..10716262R. doi: 10.1073/pnas.1005769107. ISSN 1091-6490. PMC 2941342. PMID 20805472.
- ^ Brown K, Leggat PA (20 December 2016). "Human Monkeypox: Current State of Knowledge and Implications for the Future". Tropical Medicine and Infectious Disease. 1 (1): 8. doi: 10.3390/tropicalmed1010008. PMC 6082047. PMID 30270859.
- ^ a b c Van Beusekom M (16 March 2024). "More than 600 dead in spreading DR Congo mpox outbreak as Republic of Congo reports its first cases". University of Minnesota. CIDRAP. Retrieved 19 March 2024.



